Gary Abanatha proudly served his country in the United States Army. In 2010, he received medical discharge due to issues with pain in his back, hips and neck.
Gary dealt with the pain for years, and even went to physical therapy and received injections to help alleviate his symptoms. However, even the simplest things, like walking, hurt Gary.

“Getting to the point of needing surgery was a long process,” Gary shares. “I went back and forth with a few doctors until I was seen by the team at Mercy Health – Paducah Neurosurgery.”
It was there that Gary came under the care of Brian Farrell, MD, PhD. Dr. Farrell joined our team at Paducah Neurosurgery team in 2019 and specializes in both general neurosurgery and spine surgery. Together, both Gary and Dr. Farrell decided the best path forward was a sacroiliac (SI) joint fusion procedure.
“Sacroiliac joint dysfunction is an under-recognized cause of life-limiting pain that can make walking, sleeping and even sitting difficult,” Dr. Farrell explains. “Like any surgery, we must be thorough and careful in our diagnostic approach. We benefit greatly from our collaboration with pain management to offer injections that allow us to confirm the diagnosis and avoid unnecessary surgeries.”
Dr. Farrell adds that the SI joint serves as the connection between the pelvis and the spine. A stable SI joint, combined with the surrounding muscles, keeps your pelvis and spine from moving in ways that can cause severe pain.
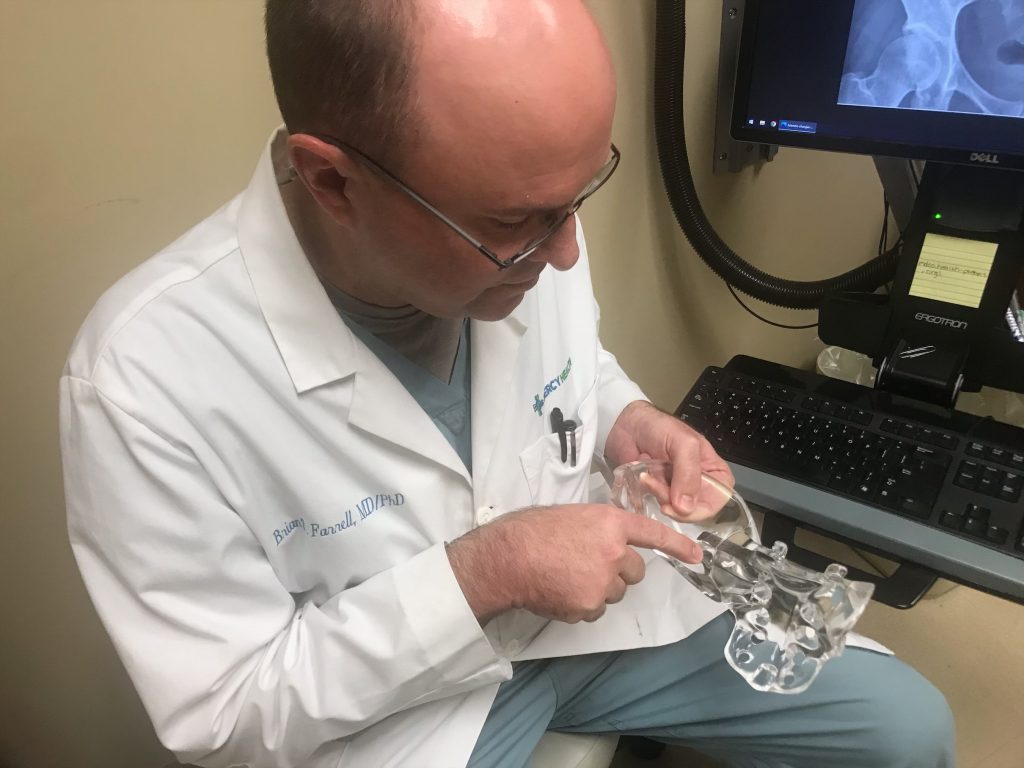
In Gary’s case, his SI joint was not working properly, which made his legs different lengths – three inches different!
“It’s almost like I didn’t have muscles left to keep my joint in place,” Gary describes. “I was standing on one foot or the other because I couldn’t stand on both feet, as my legs weren’t the same length. I was always compensating.”
In a SI joint fusion procedure, a surgeon fuses your SI joint with implants that keep it from moving.
“I dealt with my pain for so long. I got so used to it that I downplayed the pain I was experiencing day in and day out,” Gary shares. “After the surgery, I put my walker away after a week. I carried a cane for about another week. After two weeks, I was walking on my own. Some days, I don’t have pain at all.”
Dr. Farrell adds, “I’m thankful that we can offer this surgery to our patients. In patients who are properly identified, we can use a minimally invasive technique through a small incision that stabilizes the SI joint to improve both pain and function. Gary’s case went very smoothly with an excellent radiographic and clinical outcome, which is what we expect.”
Learn more about the neurosurgery services we provide at Mercy Health.