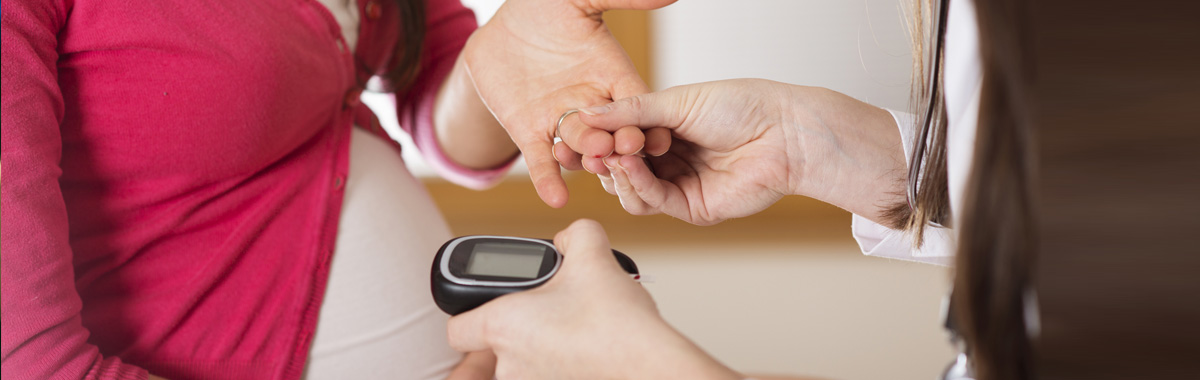
Gestational diabetes is common during pregnancy. Here’s what you need to know.
Your body goes through many changes when you’re pregnant. Sometimes you can’t make or use the insulin, a substance that helps your body process sugar, that’s necessary for pregnancy. That’s because your cells may become a resistant to insulin when you’re pregnant.
Without enough insulin in your cells, the sugar can’t leave your blood and turn into the energy you need during pregnancy. The sugar then builds up in your bloodstream and gives you gestational diabetes.
Effects of gestational diabetes
The reason you become resistant to insulin is because your body wants extra sugar as nutrition for your baby.
Gestational diabetes can be risky for your baby in the following ways:
- Extra sugar may result in a high birth weight.
- Your high blood sugar may induce early labor.
- Your baby may develop Type 2 diabetes later in life.
- Your baby may have difficulty breathing if born too early.
- A high birth weight may increase the baby’s risk of obesity later in life.
- Your baby may be born with high levels of insulin, resulting in low blood sugar and seizures.
Gestational diabetes is serious. Left untreated, it can also result in a stillborn baby or death after birth.
Can I prevent gestational diabetes?
You can’t entirely prevent gestational diabetes. The way your hormones work during pregnancy often determines if you develop insulin resistance.
To lower your risk, lose excess weight before pregnancy. You can also eat healthy foods throughout your pregnancy. Luckily, once a doctor diagnoses it, gestational diabetes can be successfully treated.
Risk factors for gestational diabetes
It’s tough to know if you’ll get gestational diabetes. However, there are a few risk factors to consider.
If you have high blood sugar before pregnancy, you may develop gestational diabetes. High blood pressure may lead to the condition. Here are a few other factors that can put you at higher risk for getting gestational diabetes:
- You’re older than 35.
- Your body mass index is 30 or higher.
- Your family has a history of developing diabetes.
If you had gestational diabetes during an earlier pregnancy, you’ll likely have it again during other pregnancies.
Symptoms of gestational diabetes
It is possible to have gestational diabetes without having any symptoms. However, your doctor will test you throughout your pregnancy to see if you’re at risk. The most important time to have checkups is during the last three months of pregnancy. This is when doctors need to test your blood sugar levels.
Some symptoms may include increased thirst and urination. Those symptoms, however, can occur during pregnancy without gestational diabetes.
Diagnosis of gestational diabetes
Doctors usually figure out if you have gestational diabetes during the second half of your pregnancy, and blood sugar level testing determines that. Testing for gestational diabetes includes quickly drinking a sugary liquid to raise your blood sugar levels. Then, doctors test your blood to see how your body processes the sugar.
If the results show that you have a high level of sugar in your blood, you’ll have more tests. You will likely need a fasting blood test and a long glucose test. Your doctor may also refer you to other specialists who can help you manage and treat your blood sugar levels during your pregnancy.
Treatments for gestational diabetes
If you have gestational diabetes, your will doctor need to monitor you as part of your treatment. You’ll need to keep your blood sugar at a normal level.
Treatments to do that include:
- Special diet
- Insulin injections
- Scheduled exercise
- Daily blood glucose testing
Keeping up with your treatment can also lower your risk of giving birth by cesarean section to a large baby.
Recovery from gestational diabetes
After childbirth, gestational diabetes typically goes away. You’ll still need monitoring during any future pregnancies. Having gestational diabetes also means you may be at risk for developing Type 2 diabetes later.
If you do have gestational diabetes, it’s a good idea to continue leading a healthy lifestyle to minimize the risks.
Are you planning on trying to get pregnant soon? Learn more about the maternity care services we provide at Mercy Health and find a provider near you.